|
Multiple cranial nerve deficits is highly suggestive of brainstem injury. *Anisocoria in the absence of orbital traumaĪbnormalities in a cranial nerve reflex indicate injury to the brainstem or the neural pathway connecting to the brainstem. Interpretation of pupil size and reactivity. In addition serial pupil examinations are one of the most useful methods for detecting changes in patient status. Important cranial nerve reflexes to evaluate include:Įxamining the pupils helps determine the nature and severity of the brain injury (Table 1). Serial neurologic examinations need to be performed in the first 24 hours as rapid changes in status can occur and will require immediate intervention if therapy is to be successful. The aim of assessment is to determine the location and severity of the injury. Neurological assessment should include evaluation of the level of consciousness, cranial nerve reflexes and skeletal motor responses. The sensitivity and specificity of this method for detecting CSF in veterinary patients has not been evaluated. 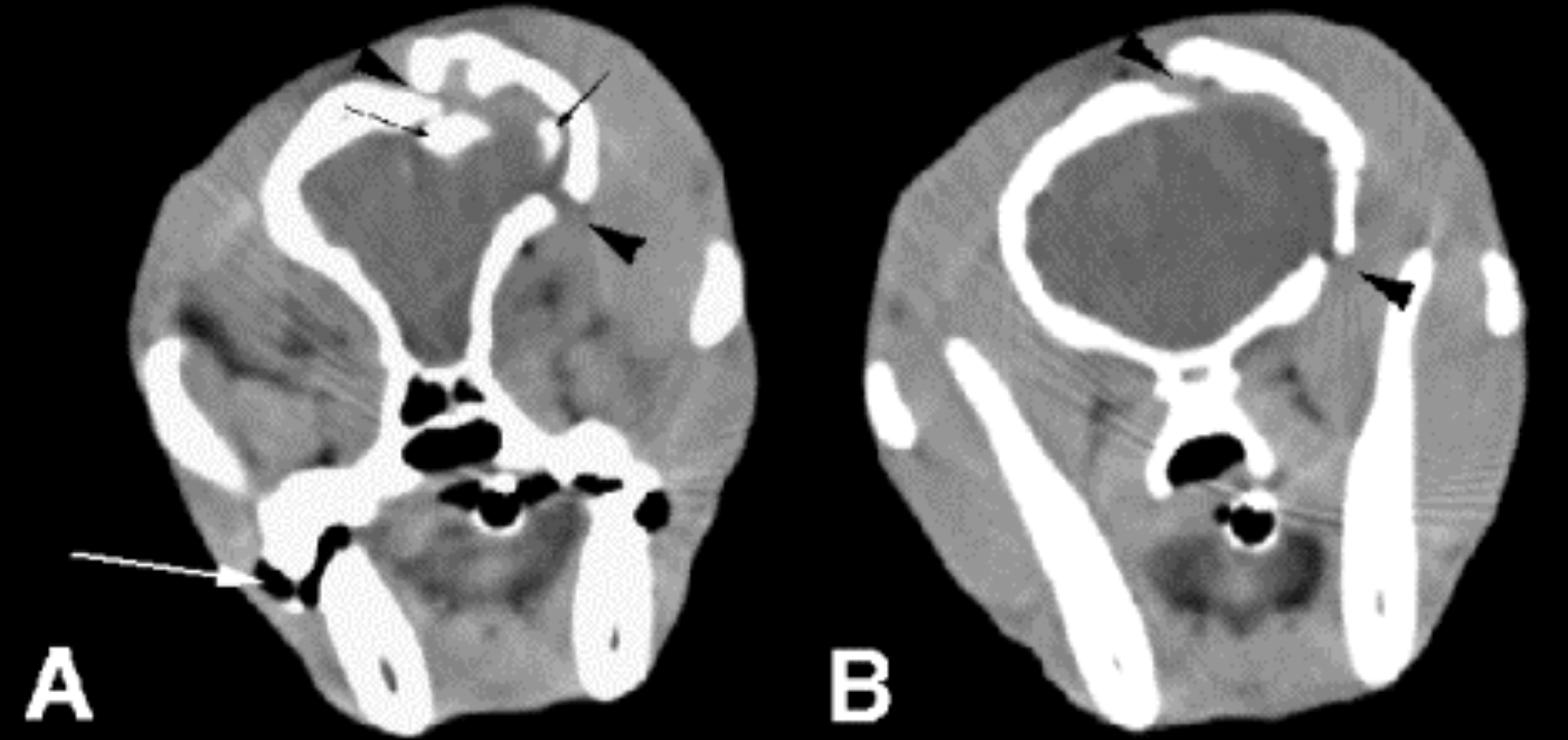
CSF has a blood glucose of ~60% of serum glucose, true nasal/aural discharges do not contain glucose. Clear fluid from the external ear canal can be collected and a blood glucose measured. 
The external ear canals are examined for the presence of blood or CSF which may indicate the presence of basilar skull fractures. Patients with head trauma may also sustain spinal trauma and should be handled cautiously until these injuries have been evaluated.Ī brief evaluation of abrasions and/or lacerations over the head is performed for evidence of decompressed or open skull fractures. The patient should be fully resuscitated before neurologic injuries are evaluated. If vasodilation occurs it can effectively increase the blood volume within the cranium and contribute to intracranial hypertension.Īs with all emergency patients the primary survey of airway, breathing and circulation should be assessed first. The PCO 2 is one of the most important determinants of cerebral blood flow. 
When autoregulation is intact, cerebral vessels will vasodilate in response to hypercapnia or hypoxemia. Hypertension in the brain trauma patient requires immediate intervention This hypertensive response is called the Cushing's reflex and is accompanied by a bradycardia. This stimulates systemic hypertension in an attempt to improve cerebral blood flow. If cerebral ischemia occurs there is a 'cerebral ischemic response'. This can cause brainstem compression and is often a terminal event. Intracranial hypertension will reduce cerebral blood flow (see below), alters neuronal function and if severe can lead to herniation of the cerebrum or cerebellum. Brain trauma patients can have increases in intracranial volume and hence pressure as a consequence of cerebral oedema, haemorrhage, vasodilation and venous outflow obstruction. 
The cranial vault is an enclosed space which contains three essential components: brain parenchyma, blood and cerebral spinal fluid (CSF). The clinician cannot alter the extent of the primary injury and instead must focus on preventing or minimising the occurrence of secondary brain injuries. Patients that survive the initial injury are at risk of deterioration and possibly death due to progressive derangements in blood flow and cellular function, a process known as secondary brain injury. Traumatic brain injury causes primary structural damage as a result of contusion, laceration, compression and/or haemorrhage of the parenchyma. Appropriate, effective management of these patients can have a dramatic impact on outcome. Traumatic brain injury is a common concern in the small animal emergency patient.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
